First Aid-Lesson 18-Envenomation
Envenomation
Envenomation refers to the process by which a bite or sting from venomous creatures such as jellyfish, snakes, spiders, and insects like bees, wasps and ants injects venom.
In Australia, where a diverse range of venomous wildlife exists, knowing how to handle envenomation is essential for safety.
In Australia, the phone number 13 11 26 is the national telephone number for the Poisons Information Centre. Available 24/7, this hotline provides immediate, expert advice on managing poisonings, drug overdoses, bites, stings, and chemical exposures.
Poisonous bites and stings from different animals require different first aid treatments. The type of animal and the nature of its venom determine the specific steps you need to take to provide effective first aid, so it’s important to know how to recognise and treat each one.
Pressure Immobilisation Technique (PIT)
The pressure immobilisation technique (PIT) is a first-aid method used to slow the spread of venom after certain bites and stings, particularly from snakes and some spiders, octopuses, and shellfish.
This technique involves applying a bandage tightly around the affected area and then immobilising the limb with a splint. The idea is to slow the venom’s movement without stopping blood flow, giving the casualty more time to get medical help.
PIT stops the venom spreading through the lymphatic system by restricting the flow of lymph and blood, without stopping arterial blood flow. PIT is used to manage bites from creatures whose venom spreads quickly through the body, but it is not suitable for all types of envenomation, such as those from jellyfish or certain other spiders.
PIT is recommended for bites and stings from:
- funnel web spider
- blue-ringed octopus
- cone shell
- all Australian venomous snakes (including sea snakes).
DO NOT
- Do NOT wash the bitten area.
- Do NOT cut or excise the bitten area.
- Do NOT attempt to suck venom from the bite.
- Do NOT use arterial tourniquets. This is a device that applies pressure to a limb to restrict (but not stop) arterial blood flow, used for controlling severe bleeding in medical emergencies or
surgeries. These are dangerous and not recommended for any bites or stings in Australia.
If resuscitation is needed, it must come before PIT. However, the resuscitation team should apply PIT as soon as they can to help slow the spread of venom
Snakebite
Snake bite and envenomation (systemic poisoning from the bite) are rare in Victoria. There are three venomous snakes in Victoria:
- Brown snake
- Tiger snake
- Red Bellied Black
Snakebite symptoms
- Fang marks
- Multiple scratches
- Painful
- Swollen
- Bruised
First aid for a venomous snake bite
The most common cause of death from a snake bite is a sudden collapse leading to cardiac arrest. This severe reaction can happen quickly, usually within 10 to 60 minutes after the bite, often before the victim reaches a hospital. Immediate CPR is essential in such cases to try to save the person’s life.
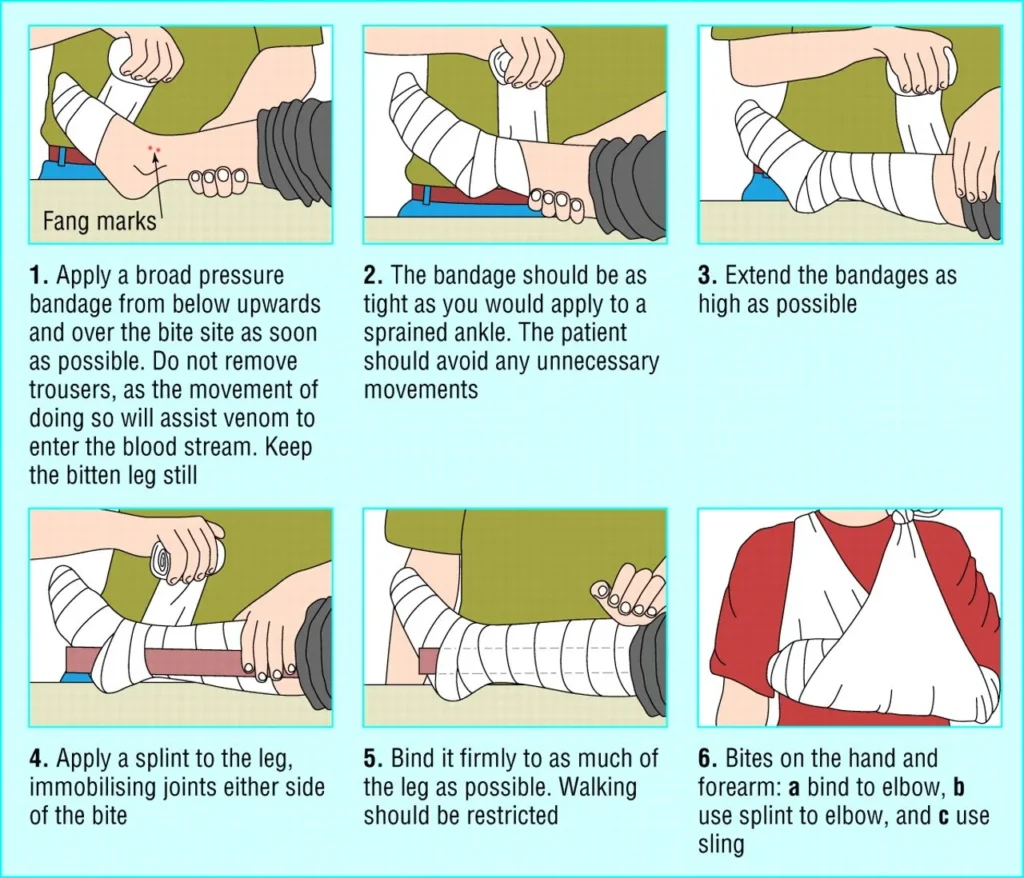
Apply a broad pressure immobilisation bandage, preferably elastic rather than crepe, as firm as you would for a sprained ankle; the aim is to prevent lymphatic spread of venom, not to stop blood supply.
- Start at the bite site and bandage the entire limb.
- Immobilise the joints on either side of the bite site (use a splint),
Immobilise the entire child as well (lay the child down). - DO NOT remove the bandage until you are in a centre with full treatment facilities, as discussed above.
- If envenomed, do not remove the venomous material until antivenom has been administered.
- Once the antivenom has been given, remove the pressure immobilisation bandage.
- Do not wash or clean the bite site in any way (in case a Venom Detection Kit is required).
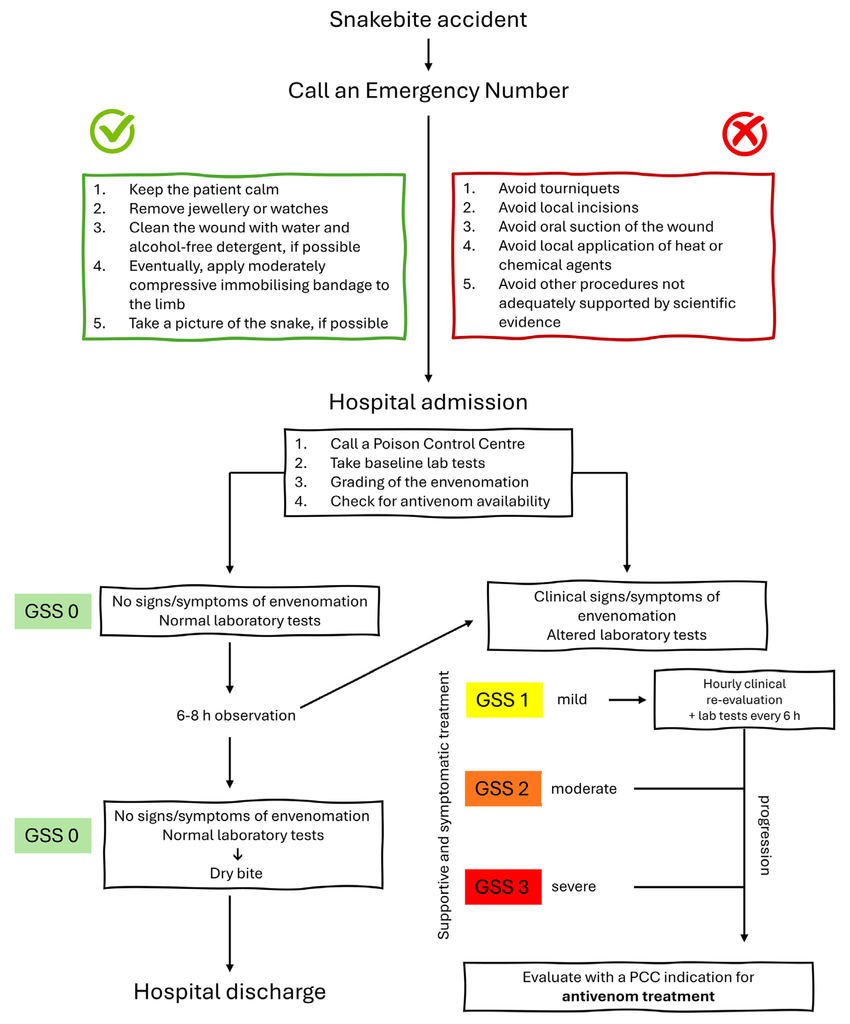
Spider bites
In Australia, many spider bites can be painful, but most spider bites are non-lethal and may only
cause minor symptoms like redness, itching or minor pain. However, bites from funnel web spiders
can be lethal, and the redback spider bite can be serious and even life-threatening for very
young or very old people.
First aid for spider bites
The treatment/management for funnel web spider bites follows the same steps as for venomous snakes, using the pressure immobilisation technique to slow down the spread of venom.
Once at a medical facility, antivenom is often administered to counteract the venom. This is the most effective treatment for severe symptoms and should only be administered in a
hospital setting.

- Wash the bite area and keep it clean to avoid infection.
- Use an ice pack or cold compress on the affected area to reduce pain, but not for more than
20 minutes at a time. - Continuously monitor the person.
- Arrange for the person to be transported to a medical facility, by ambulance if possible,
especially if it involves a young child, if there is a collapse, or if the pain is severe. - Do NOT use the pressure immobilisation technique.

The treatment for other spider bites, including the white-tailed spider bites, is relatively straightforward. You should apply an ice pack to the bite area to help relieve pain. Note that white- tailed spider bites can cause severe inflammation, but they are not known to cause severe tissue
damage. If the symptoms are more serious or the person feels very unwell, it’s advised to seek medical attention.

Tick bites
Tick bites in Australia generally don’t cause significant symptoms in most cases. However, in some individuals, tick bites can lead to severe allergic reactions or anaphylaxis, which is potentially life-threatening. The paralysis tick is particularly notorious in Australia for causing severe reactions, including paralysis.
| Signs and symptoms of tick bites | Paralysis tick bites |
|---|---|
| – Immediate and intense pain at the site of the bite.
– Local redness and swelling. – In cases of severe allergic reaction, symptoms can include difficulty breathing, swelling of the face and tongue, abdominal pain, vomiting and a generalised rash. |
The initial signs and symptoms of a paralysis tick bite can be subtle but may progress to more serious conditions if the tick remains attached and continues to inject toxin.
– Local irritation and redness at the bite site. – Mild to severe allergic reactions. – Progressive symptoms can include weakness, – Facial paralysis or an inability to move parts of the face. – In severe cases, difficulty in breathing due to |
First aid for tick bites
| Step 1 | If the person is not responding or not breathing normally, you should start CPR and call 000. |
| Step 2 | If the person isn’t allergic to ticks, it’s important to kill the tick quickly to reduce the risk of developing an allergy. If the person is allergic to ticks, make sure you don’t try to remove the tick; kill it where it is. |
| Step 3 | Begin by using an ether-containing spray, available over the counter at pharmacies, to kill the tick. Position the spray about 1cm above the tick and apply it 5 times. |
| Step 4 | Wait around five minutes for the tick to die and fall off. You can check if the tick is still alive by observing its legs with a magnifying glass; if the legs aren’t moving, the tick is dead. If you don’t have a magnifying glass or if the tick is still alive, spray it again 5 times |
| Step 5 | If the person isn’t allergic to ticks, it’s important to kill the tick quickly to reduce the risk of developing an allergy. If the person is allergic to ticks, make sure you don’t try to remove the tick; kill it where it is. |
| Step 6 | Once the tick has been killed and removed, you can use a cold compress to reduce the swelling and pain. |
Bee and wasp stings
Bees
In Australia, the most commonly known stinging bee is the introduced European honey bee. When threatened, these bees can sting, leaving behind a barbed stinger that causes them to die shortly
after.
Most native Australian bees, on the other hand, are generally stingless. There are over 1,500 species of native bees in Australia, and most don’t sting. However, some native bees can sting, but they are usually less painful and less harmful than the European honey bee, like the blue-banded bee and the carpenter bee.
In Australia, the bee most commonly known to sting is the European honey bee, which is not native
to Australia.
Wasps
Australia is home to a diverse range of wasp species, many of which are capable of stinging. Not all wasps in Australia sting, but those that do can be broadly categorised into two groups: social and solitary wasps.
Social wasps include species such as the introduced European wasp, known for its painful sting and aggressive behaviour, especially near food sources or when their nests are disturbed. Paper wasps are also common in Australia. They are less aggressive than European wasps but will sting if threatened. Solitary wasps generally don’t sting humans unless provoked and spend most of their time alone, except when mating.
The European wasp is an invasive species in Australia, known for its aggressive behaviour and
tendency to sting when threatened. It can sting multiple times and does not lose its stinger.
| Often, the first indication of a bee or wasp sting is a sharp, sudden pain at the site of the sting.
The area around the sting usually becomes red and swollen. This swelling can increase over hours and sometimes affects a larger area. As the initial pain subsides, the sting site may become itchy, a condition that can last for several days. The area around the sting may feel warm to the touch due to inflammation. At the sting site, you might notice a small white spot where the stinger punctured the skin. |
Often, the first indication of a bee or wasp sting is a sharp, sudden pain at the site of the sting.
The area around the sting usually becomes red and swollen. This swelling can increase over hours and sometimes affects a larger area. As the initial pain subsides, the sting site may become itchy, a condition that can last for several days. The area around the sting may feel warm to the touch due to inflammation. At the sting site, you might notice a small white spot where the stinger punctured the skin. |
First aid for bee and wasp stings
| Stinger removal | When bees sting, their stingers detach.
If the stinger is still in the skin, it should be removed as quickly as possible to prevent more venom from being injected. Use a flat, dull edge, such as a credit card or a fingernail, to scrape it out from side to side. Avoid using tweezers or pinching the stinger, as this can squeeze more venom into the skin. |
| Clean the area | Wash the sting site with soap and water to remove any contaminants that could cause infection. |
| Apply ice or a cold pack | This helps reduce swelling and pain. Apply a cold pack to the area for a few minutes at a time. |
| Pain relief | Over-the-counter pain relievers like paracetamol or ibuprofen can be used to manage pain. |
| Topical treatments | Applying hydrocortisone cream or calamine lotion can help soothe the skin and reduce itching. |
| Antihistamines | If someone has a history of severe allergic reactions to bee stings, they should carry an adrenaline autoinjector (e.g., EpiPen) and know how to use it.
If symptoms of anaphylaxis appear, administer adrenaline and call for emergency medical help immediately. For non-allergic individuals, bee and wasp stings are usually a minor irritation that resolves within a few hours to a few days, whereas for those with allergies, it’s essential to be prepared to respond promptly to severe reactions. |
| Monitor for allergic reactions | If the sting causes significant itching, oral antihistamines may help reduce the reaction. |
| Anaphylaxis | If someone has a history of severe allergic reactions to bee stings, they should carry an adrenaline autoinjector (e.g., EpiPen) and know how to use it.
If symptoms of anaphylaxis appear, administer adrenaline and call for emergency medical help immediately. For non-allergic individuals, bee and wasp stings are usually a minor irritation that resolves within a few hours to days, whereas for those with allergies, it’s essential to be prepared to respond to severe reactions promptly. |
The symptoms and initial treatment of bee and wasp stings are similar, but there are a few key differences to be aware of.
| Pain and venom | Both bee and wasp stings cause sharp pain and deliver venom that can cause an immediate skin reaction. However, wasp venom can cause a more pronounced inflammatory response, resulting in more intense pain and swelling. |
| Sting mechanism | Bees generally sting only once as their stinger becomes lodged in the skin and detaches from their body, leading to their death. Wasps, on the other hand, can sting multiple times without losing their stinger, potentially leading to multiple injections of venom. |
| Reaction severity | The potential for severe allergic reactions, including anaphylaxis, exists with both bee and wasp stings. However, multiple stings from a wasp can increase the severity of the reaction more significantly due to multiple doses of venom. |
| Symptom management |
The management of symptoms for both stings involves cleaning the area, applying ice to reduce swelling, and taking pain relievers. If the stinger is left in the skin (more common with bee stings), it should be scraped away. |
| Allergic reactions | Individuals who are allergic to insect stings should carry an adrenaline auto-injector (e.g., EpiPen) as they are at risk of developing severe reactions from either type of sting. |
Ant bites and stings
In Australia, ant bites and stings can vary widely in severity depending on the species.
| Bull ants | Known for their aggressive nature and powerful sting. Bull ants can cause significant pain and a strong localised reaction. In sensitive individuals, their sting can trigger allergic reactions. |
| Green ants | Found primarily in tropical areas, green ants deliver a sting that can be quite painful and may leave the area around the sting itchy and swollen. |
| Fire ants | An invasive species that is a significant concern in parts of Queensland. Fire ant stings can be very painful and often result in a raised welt that can become itchy. |
| Jack jumper ants | An invasive species that is a significant concern in parts of Queensland. Fire ant stings can be very painful and often cause a raised welt that may become itchy. |
Symptoms of an ant bite
- Pain is usually the first and most immediate symptom. Stings from ants like the bull ant or jack jumper can be particularly painful.
- The area around the bite or sting typically becomes red and swollen. Swelling can be more extensive depending on the individual’s reaction to the ant’s venom.
- As the initial sharp pain subsides, itching often develops and can last for several days.
- After a fire ant sting, small blisters may form at the sting site. These blisters are distinctive, often looking like a white pustule on a red base.
- While less common, some individuals may experience severe allergic reactions to ant stings, which could include symptoms such as difficulty breathing, dizziness, a rapid increase in heart rate and swelling of the face, lips, or throat. These symptoms require immediate medical attention.
First aid for an ant bite or sting
| Clean the area | Immediately wash the bite or sting area with soap and water to remove any ant venom residue, which can help in reducing the severity of the reaction. |
| Cold compress | For severe itching or a known mild allergy to ant stings, an oral antihistamine may help reduce the reaction and provide relief. |
| Topical treatments | Use over-the-counter creams such as hydrocortisone or a calamine lotion to relieve itching and discomfort. These can help minimise the reaction and soothe the skin. |
| Pain relief | If the pain is significant, over-the-counter pain relievers like paracetamol or ibuprofen can be used according to the product instructions. |
| Avoid scratching | Encourage the person not to scratch the bite site. Scratching can increase irritation, prolong healing and lead to infection. |
| Antihistamines | For severe itching or if there’s a known mild allergy to ant stings, an oral antihistamine may help reduce the reaction and provide comfort. |
| Allergic reaction monitoring | Watch for signs of a more serious allergic reaction, such as swelling of the face, lips or tongue, difficulty breathing, or a rapid spread of redness. If any of these occur, seek medical attention immediately. |
Jellyfish sting
Jellyfish stings are a common hazard for beachgoers in Australia, particularly in tropical and subtropical regions. Jellyfish stings occur when thousands of tiny stinging structures called nematocysts, found on jellyfish tentacles and sometimes on their bodies, release venom-filled tubules into the skin.
In Australia, there are many types of jellyfish, including the potentially deadly box jellyfish, which is mainly found in northern Australia and is known for its extremely painful, life-threatening stings. Other species, like the bluebottle (or Portuguese man o’ war), are less dangerous but can still cause
painful stings that result in redness, swelling, and intense pain at the site of contact.
The severity of a jellyfish sting depends on the species, the amount of venom injected and the individual’s reaction. The more tentacles that touch the skin, the more venom is injected. Severe stings are most common in tropical regions and pose greater risks to children due to their smaller body size.
Symptoms of jellyfish stings
| Skin markings | Jellyfish stings can leave a variety of skin markings that vary based on the species involved. Here are some types of skin reactions you might see: Subtle markings: these may start as barely noticeable marks that can develop a red flare or take on an appearance similar to goosebumps or an orange-peel texture. Some marks may also show profuse sweating localised to the sting area. Blotchy and wheal reactions: you might see irregularly shaped blotchy areas or raised, white wheals surrounded by red flares. Distinctive patterns: multiple linear, whip-like wheals or a pattern resembling a frosted ladder are indicative of a box jellyfish sting, which is known for more severe reactions. Progression of symptoms: the initial marks can later blister or darken as the sting site reacts over time. |
| Pain | Pain is typically immediate upon stinging.
Intensity varies from mild irritation to severe, sharp, or burning sensations. Generalised muscle aches are common. Severe muscle cramps can occur in the limbs, chest and abdomen. |
| Severe jellyfish stings |
Difficulty breathing or stopping breathing.
Potential for cardiac arrest. Intense pain that may be continuous. Behaving in a restless or irrational way. Nausea and vomiting, accompanied by headaches. Physical collapse. Heavy sweating, often localised to the area around the sting. |
First aid for a jellyfish sting
First aid for bluebottle jellyfish stings
- Wash the sting site with seawater (not fresh water)
- Remove any tentacles by hand or wash them off with seawater
- Put the affected limb in hot water (45ºC) for 20 minutes; make sure the hot water will not burn you
If you can’t put the limb in hot water, try a hot shower or running hot water over the sting site. Hot water is better than ice packs at reducing the pain of bluebottle jellyfish stings.
Do NOT put vinegar on the sting. It may increase the pain of bluebottle jellyfish stings.

First aid for other jellyfish stings
- Wash the sting site with seawater (not fresh water)
- Remove any tentacles by hand or wash them off with seawater
- Consider putting your affected limb in hot water (45ºC) for 20 minutes — make sure the hot water will not burn you
Do NOT put vinegar on the sting. It may increase your pain.
First aid for Irukandji Syndrome
If you think someone has Irukandji syndrome, take the casualty to the hospital.
In the hospital, the casualty may be given intravenous (IV) pain medication. They will also check whether the jellyfish sting has affected the casualty’s heart.

First aid for other major box jellyfish stings
If the person is unconscious, do CPR.
First aid for a major box jellyfish sting involves:
- Removing any tentacles by hand or washing them off with seawater (not freshwater)
- Once the tentacles are removed, putting vinegar on the sting site — vinegar deactivates the stinging cells
- Using ice packs
- Go to a hospital

Expanded Learning Materials
Expanded
Learning
Materials