First Aid – Lesson 6 – Allergy, asthma & hay fever
Severe allergic reactions (anaphylaxis) and asthma attacks related to allergies need emergency first aid. If you (or a family member) have previously had asthma or a severe allergic reaction, prepare an action plan with the help of your doctor. Follow the plan if the symptoms of an allergic reaction appear.
Allergic symptoms
Symptoms of a severe allergic reaction (anaphylaxis) include:
- Difficult or noisy breathing
- Swelling of the tongue
- Swelling or tightness of the throat
- Difficulty talking or a hoarse voice
- Wheeze or persistent cough
- Persistent dizziness or collapse
- Paleness and floppiness in young children
- Abdominal pain and vomiting.
Milder allergic symptoms that can appear before a severe allergic reaction include:
- Swelling of your lips, face and eyes
- Hives or welts
- Tingling mouth
- Abdominal pain and vomiting.
If you have experienced any of these symptoms, you are at greater risk of having another severe reaction. Ask your doctor to refer you to a medical specialist (allergist or clinical immunologist).
First aid for severe allergic reactions
A severe allergic reaction (anaphylaxis) is life-threatening and requires urgent action. Emergency responses for severe allergic reaction (anaphylaxis) are:
- Reassured casualty
- Lay the patient down.
- If breathing difficulty is present, the patient should be placed in the upright position
- Located EpiPen and anaphylaxis action plan, followed instructions according to plan
- Checked expiry, name and “Window”.
- Administered EpiPen in the outer thigh, held for 10 seconds, rubbed the site, stored EpiPen safely, and recorded the time given.
- Call 000
- Continued to monitor the patient. Administer a second EpiPen if available after 5 minutes if there is no improvement or the condition deteriorates
- Continued to monitor and reassure the patient
- Prepared to administer CPR if the patient became unconscious, unresponsive and not breathing
- Report details of the incident to the workplace First Aider and the Ambulance officer as required
Adrenaline autoinjectors
Adrenaline works fast to reverse a severe allergic reaction, and adrenaline autoinjectors (EpiPens®) are designed for use by people who are not medically trained. If you are at risk, your doctor will have prescribed an adrenaline autoinjector.
- In an emergency, we always use EpiPens® for adults and children.
- However, for children weighing 15 kg to 30 kg, we choose EpiPen Jr (150 mcg).
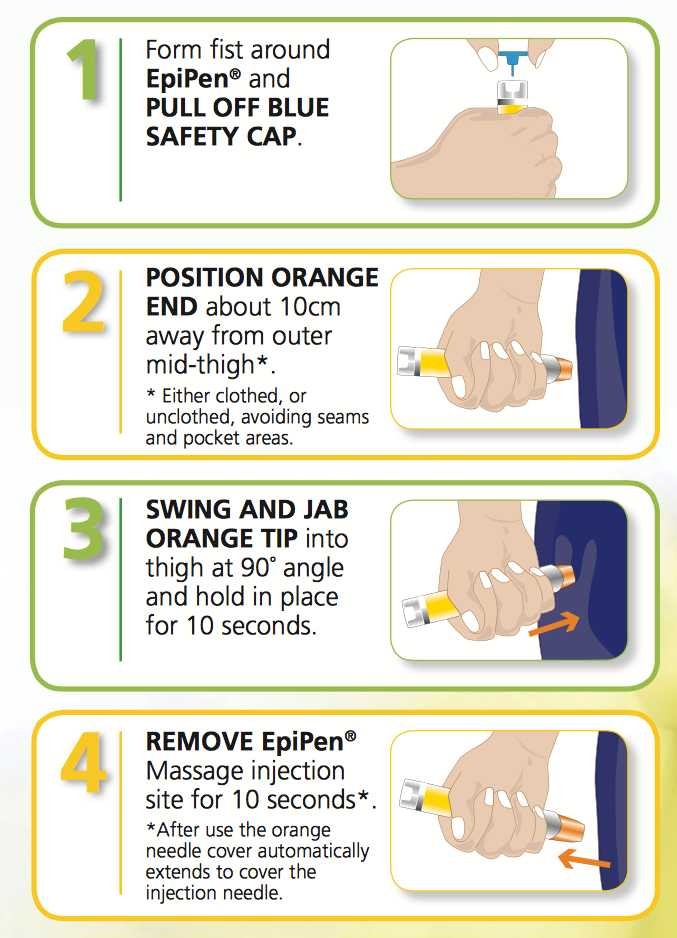
Adrenaline works fast to reverse a severe allergic reaction, and adrenaline autoinjectors (EpiPens® are designed for use by people who are not medically trained. If you are at risk, your doctor will have prescribed an adrenaline autoinjector.
Asthma
Asthma is defined as a chronic (Long-term) lung disease that inflames and narrows the airways. It is usually related to an allergic reaction or hypersensitivity.
Asthma affects one in ten Australians. Causes of asthma are not exactly known; there are a number of contributing factors, which include:
- Family history of asthma
- Eczema
- Hay fever
- High pollen count in the environment
- Weather
- Air pollution
- Exposure to allergens
- Smoking
If you have asthma, your doctor will prescribe the correct medication and help you to develop a plan to manage your asthma and an action plan for asthma attacks. Asthma can be well controlled with medication in most people.
The signs of asthma include when the person:
- Wheezing
- Chest tightness
- Coughin
- Finds it very difficult to breathe
- Is unable to speak comfortably, or if their lips are turning blue
- Has symptoms that get worse very quickly
- Is getting little or no relief from their reliever inhaler.
The following reasons may trigger an asthma flare-up.
- Pollen
- Molds
- Animals
- Certain foods
- Feathers
- Smoking
- Dust
The main types of medication are:
- Relievers that act quickly to relax the muscles around the airways – this is the medication used during an asthma attack
- Preventers that slowly make the airways less sensitive to triggers and reduce inflammation inside the airways – they are taken daily to help keep you well
- Combination therapies that are preventers containing two different medications.
- If you, or someone you know, are having an asthma attack, follow the asthma action plan. In case of emergency, call triple zero (000) and ask for an ambulance. Tell the operator that someone is having an asthma attack.
While waiting for the ambulance, give four puffs of reliever medication every four minutes.
If the person having the asthma attack (or sudden breathing difficulty) is known to have an allergy to food, insects, or medication, always give the adrenaline autoinjector first, and then the asthma relief medication – even if there are no skin symptoms.

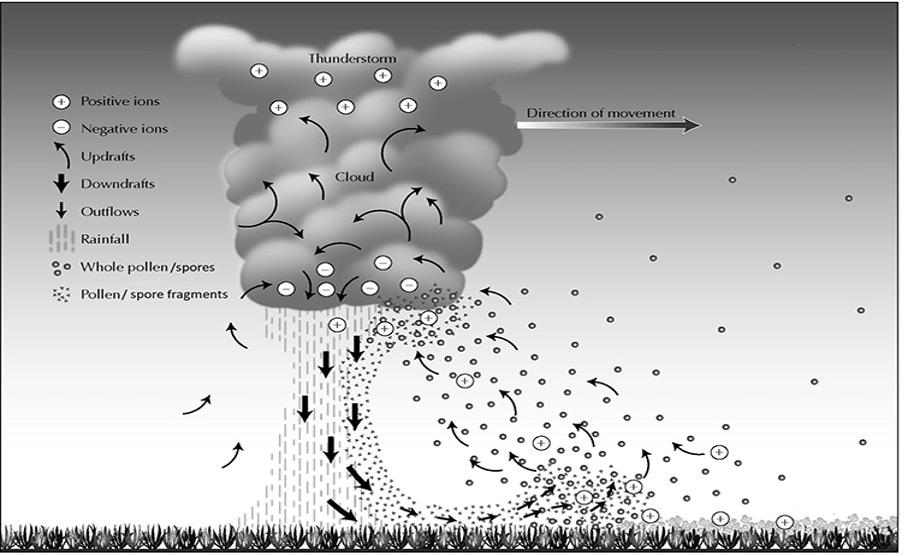
Thunderstorm asthma
By the last weekend of September, you should be taking your hay fever nasal spray, asthma preventer, or both – and you shouldn’t stop until New Year’s Day (most adults with asthma do need to take a preventer all year, not just in springtime).
Thunderstorm asthma can happen suddenly to people in spring or summer when there is a lot of pollen in the air, and the weather is hot, dry, windy, and stormy.
People with asthma and/or hay fever need extra protection to avoid thunderstorm asthma between September and January in Victoria, New South Wales and Queensland. This means using preventer medicine every day and always having a reliever inhaler (blue puffer) ready. See your doctor to get the best asthma and/or hay fever medication plan.
Spring thunderstorm weather can cause pollen grains to burst into tiny pieces, and the wind then blows them around us. When people inhale these tiny pollen particles, they can reach deep into the lungs, triggering an asthma attack.
Spring weather can also cause breathing problems for people with seasonal hay fever. People who wheeze and sneeze with hay fever from pollens during spring are more likely to get thunderstorm asthma even if they haven’t had asthma before.
November 2016: Victorian thunderstorm asthma event
On Monday, 21 November 2016, severe thunderstorm activity in Victoria led to thousands of people suddenly having asthma attacks and finding it hard to breathe. Because so many people needed urgent asthma treatment at one time, it was hard for ambulance and hospital emergency rooms to help everyone.
People are more likely to get thunderstorm asthma
- Those who get asthma and seasonal hay fever
- Those with hay fever who have never had asthma
- Those with past asthma or unrecognised asthma
Hay fever
If you already have springtime hay fever, you could suddenly get an asthma attack if you are outside in gusty wind during a thunderstorm in a place where there is ryegrass pollen in the air (most of south-eastern Australia). This can happen even if you don’t have asthma. The risk is highest between October and the end of December.
If you have asthma and pollen allergy, you could have a severe asthma attack if you are outside in gusty winds during a springtime thunderstorm in a place where there is ryegrass pollen in the air (most of south-eastern Australia).
What you can do to keep safe
- Stay up to date with pollen counts and weather forecasts during spring and early summer so you know if a storm is coming.
- Just before and during storms with wind gusts, get inside a building or car with the windows shut and the air conditioner switched to recirculate/recycled.